
Knowing F.A.S.T. is not enough; in a real crisis, the standard advice has critical gaps that can cost a life.
- Posterior strokes, which affect balance and vision, are often missed by the F.A.S.T. acronym.
- The ‘Bystander Effect’ means someone must be specifically assigned to call 911, or no one will.
Recommendation: Learn to think like a paramedic: identify specific symptoms, give direct commands, and provide critical information to ensure the right help arrives.
The moment freezes. A family member, laughing a second ago, suddenly looks confused, stumbles, or slurs their words. Panic sets in. Your mind races, grasping for a plan. Most people have heard the advice: “Remember F.A.S.T.” and “Call 911.” It’s a good start, but as a paramedic instructor, I can tell you it’s dangerously incomplete. Those simple rules are filled with critical gaps—gaps where precious minutes and brain cells are lost.
What if the stroke isn’t in the front of the brain and doesn’t affect the face or arms? What if the 911 call you make gets you a basic ambulance when you need an advanced one? What if everyone in the room assumes someone else is taking charge? These are not “what-ifs”; they are common, real-world failures in civilian emergency response. The difference between a good outcome and a devastating one often lies in navigating these gaps with the clarity and authority of a trained professional.
This is not another article that just tells you to call for help. This is your first lesson in thinking like a first responder. We will break down the paramedic’s mindset for a stroke emergency. You will learn not just what to do, but precisely why and how to do it. We’ll move beyond F.A.S.T., teach you how to talk to dispatch, clarify the critical difference between a heart attack and cardiac arrest, and show you how to take command of a scene to ensure action is taken. This is the protocol to save a life.
This guide provides the essential protocols for recognizing and responding to a medical emergency, turning a bystander into an effective first responder. The following sections break down the critical steps, from identifying complex stroke symptoms to taking decisive action before help arrives.
Table of Contents: How To Recognize Stroke Protocols To Act Within The Golden Hour?
- Why Knowing “FAST” Is Not Enough For Posterior Strokes?
- How To Speak To Dispatch To Ensure An ALS Ambulance Arrives?
- Chew or Swallow: What Is The Correct Aspirin Protocol For Chest Pain?
- The Hesitation That Kills: Why You Must Point To A Specific Person To Call 911
- What Information Must You Give The Paramedics Upon Arrival?
- Why Chest Pain Always Trumps A Broken Arm In Triage?
- Why Confusing A Heart Attack With Cardiac Arrest Delays The Right Response?
- How To Use An AED To Save A Life Before The Ambulance Arrives?
Why Knowing “FAST” Is Not Enough For Posterior Strokes?
Listen up. The F.A.S.T. acronym (Face, Arm, Speech, Time) is a decent public health tool, but it’s a blunt instrument. It primarily identifies strokes in the anterior (front) circulation of the brain. The problem? A significant number of strokes occur in the posterior circulation, which supplies the cerebellum and occipital lobe—the parts of the brain that control balance and vision. These strokes are often missed by a simple F.A.S.T. check, leading to catastrophic delays in treatment.
A person having a posterior stroke may not have face drooping or arm weakness. Instead, they might complain of sudden, severe dizziness (vertigo), loss of balance, or vision problems like double vision or blurriness. They might say, “The room is spinning,” or be unable to stand without falling. Because these symptoms are less “classic,” they are tragically dismissed as a migraine, an inner ear issue, or even intoxication. This is a fatal mistake. You must upgrade your diagnostic toolkit to include “B.E.-F.A.S.T.” where ‘B’ stands for Balance and ‘E’ for Eyes.
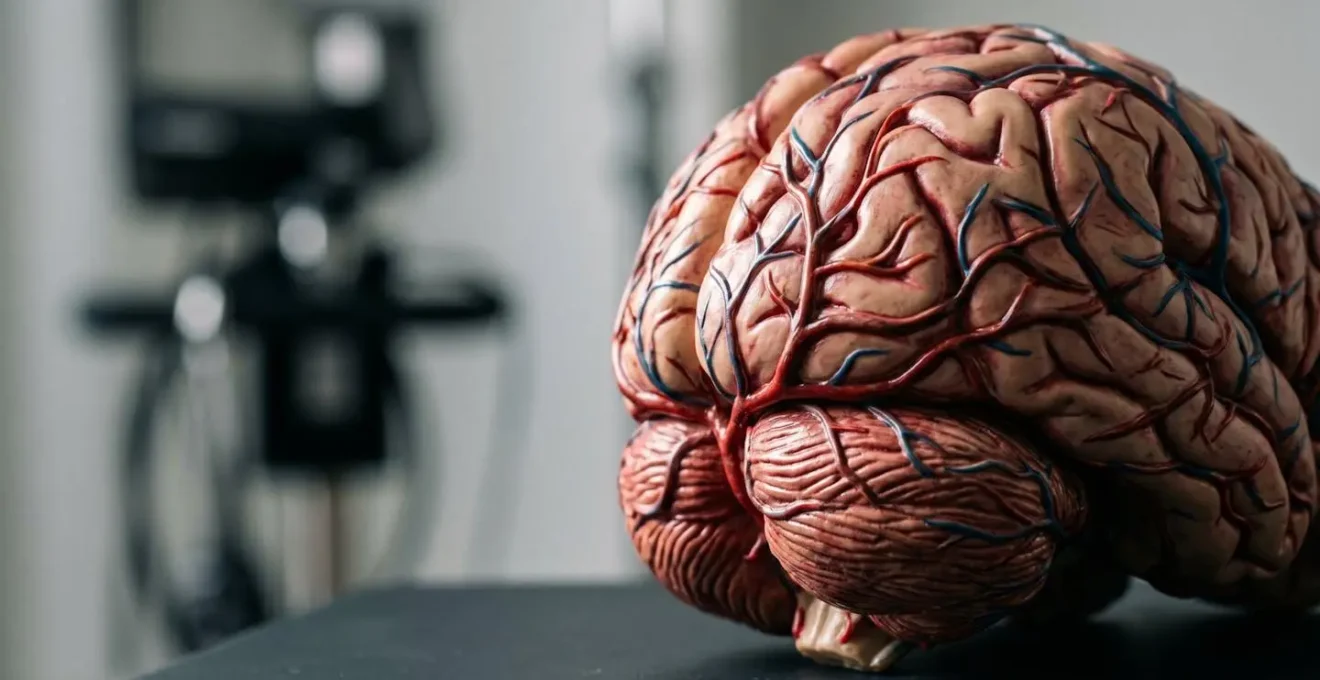
As the anatomical model shows, the blood vessels feeding the back of the brain are distinct. A blockage here produces a different set of warnings. Asking about balance and vision is not optional; it’s a critical part of a modern stroke assessment. If you see sudden balance or eye issues, with or without classic F.A.S.T. signs, you must treat it as a stroke emergency until proven otherwise.
Your Checklist: BE-FAST Enhanced Stroke Detection
- Balance: Ask ‘Are you dizzy or is the room spinning? Can you stand without assistance?’ Observe for sudden stumbling or inability to walk straight.
- Eyes: Test vision. Ask ‘Is your vision blurry? Do you see double?’ A sudden loss of vision in one or both eyes is a red flag.
- Face: Ask the person to smile wide. Look for any drooping or asymmetry on one side of the face.
- Arm: Have them raise both arms straight out in front of them for 10 seconds. Watch to see if one arm drifts downward.
- Speech: Ask them to repeat a simple, clear sentence like ‘The sky is blue today.’ Listen for slurred or strange-sounding speech.
- Time: If you see any of these signs, note the exact time they started and call emergency services immediately.
How To Speak To Dispatch To Ensure An ALS Ambulance Arrives?
You’ve identified a possible stroke. Now comes the single most important phone call you will make. How you communicate in the next 30 seconds determines the level of care that arrives at the door. Not all ambulances are created equal. There’s Basic Life Support (BLS) and Advanced Life Support (ALS). A BLS unit is staffed by EMTs who can provide oxygen and transport. An ALS unit is staffed by paramedics who can establish IVs, administer a wide range of life-saving drugs, and perform advanced cardiac monitoring. For a stroke, you need an ALS unit, period.
Dispatchers use a priority system based on keywords. You must use the magic words. Your job is to be clear, concise, and authoritative. Do not say, “My husband feels funny.” Say, “I am reporting a suspected stroke emergency.” State your location clearly. State the key symptoms you observed using the B.E.-F.A.S.T. model. Before you hang up, confirm they are dispatching an ALS unit. “Can you confirm an advanced life support unit is en route?” This isn’t being rude; it’s being a responsible advocate for the patient.
Understanding the difference in capabilities is crucial. A paramedic can notify the receiving hospital’s stroke team from the field, saving critical minutes upon arrival. They can manage blood pressure and other vitals that are crucial in an acute stroke. A BLS unit simply cannot do this. The table below outlines why your choice of words on the phone has a direct impact on the medical care the patient will receive before even reaching the hospital.
| Capability | BLS (Basic Life Support) | ALS (Advanced Life Support) |
|---|---|---|
| Personnel | EMT-Basic trained responders | Paramedics with advanced training |
| Cardiac Monitoring | Basic vital signs only | Advanced cardiac monitoring (12-lead ECG) |
| IV Access | Not authorized | IV line placement and fluid administration |
| Medication Administration | Limited to oxygen, aspirin | Wide range of emergency medications including stroke protocols |
| Airway Management | Basic airway support | Advanced airway management including intubation |
| Stroke Protocol | Recognition and transport only | Pre-hospital stroke assessment, notification to receiving hospital |
Chew or Swallow: What Is The Correct Aspirin Protocol For Chest Pain?
This is where wires get crossed with deadly consequences. People hear “aspirin” and “emergency” and make a fatal assumption. Let me be crystal clear: You only consider giving aspirin for a suspected heart attack, NEVER for a suspected stroke. A heart attack is a plumbing problem—a blockage in the heart’s arteries. Aspirin helps by making platelets less sticky, potentially reducing the clot. A stroke can be caused by a clot (ischemic) or a bleed (hemorrhagic). If you give aspirin to someone having a hemorrhagic stroke, you can make the bleeding in their brain catastrophically worse.
So, rule one: If the primary symptoms are from the B.E.-F.A.S.T. list—face drooping, arm weakness, speech difficulty, balance or vision loss—aspirin is off the table. Do not touch it. If, however, the primary symptom is crushing chest pain, pressure, or tightness, often radiating to the arm, jaw, or back, you are likely dealing with a heart attack. In this specific scenario, and only after calling 911, aspirin can be a life-saving bridge until paramedics arrive. The method is just as important as the decision. Do not have the person swallow the pill with water. They must CHEW it thoroughly. Chewing allows the aspirin to be absorbed much faster through the mucous membranes in the mouth (buccal absorption), getting it into the bloodstream where it’s needed.
Your Checklist: Aspirin Administration for Suspected Heart Attack
- Verify Symptoms: Confirm it is chest pain (pressure, tightness, radiating to arm/jaw), NOT stroke symptoms. Look for shortness of breath, nausea, or sweating.
- CRITICAL: NEVER give aspirin for stroke symptoms (face droop, speech difficulty). It can be deadly in a bleeding stroke. If in any doubt, do not give it.
- Dose: Use one 325 mg non-enteric-coated (uncoated) adult aspirin OR four 81mg low-dose (“baby”) aspirins.
- Method: Instruct the person to CHEW the aspirin completely before swallowing. Do not just swallow it whole.
- Timing: Note the exact time the aspirin was given. Write it down.
- Communication: Inform the 911 dispatcher and arriving paramedics that aspirin was given, stating the dosage and the time.
The Hesitation That Kills: Why You Must Point To A Specific Person To Call 911
An emergency unfolds in a public space. A person collapses. A crowd gathers. Everyone looks concerned, everyone knows someone should call 911, but no one moves. Seconds tick by. This is not because people are uncaring; it’s a well-documented psychological phenomenon called the “Bystander Effect” or diffusion of responsibility. When a group of people witnesses an emergency, each individual assumes someone else will intervene. The result? No one does.
As research has shown, the more people present, the less likely any single individual is to help. In fact, some psychological research indicates an over 50% likelihood drop in intervention with more than five bystanders present. The only way to shatter this paralysis is with a direct, personal command. Do not shout to the crowd, “Somebody call 911!” This is an invitation for inaction. You must take command of the scene. Make eye contact with one single person. Point at them. Use a clear, identifying feature. “You, in the red jacket. Call 911 now. Tell them we have a possible stroke. Report back to me when it’s done.”

That single, decisive action does three things: It breaks the diffusion of responsibility, it assigns a specific task, and it creates accountability. You have now deputized an assistant. You can then assign other tasks: “You, go find the building’s AED,” or “You, please clear some space for them.” This concept isn’t new; it’s a cornerstone of crisis management, first widely studied after a tragic and infamous case.
The bystander effect was first demonstrated and popularized in the laboratory by social psychologists John M. Darley and Bibb Latané in 1968 after they became interested in the topic following the murder of Kitty Genovese in 1964.
– Research by Darley and Latané, Wikipedia: Bystander Effect
What Information Must You Give The Paramedics Upon Arrival?
When we walk through that door, the scene is chaotic. Our first job is to cut through the noise and get to the signal. We need specific information, and we need it now. Every minute we spend trying to piece together the story is a minute lost for treatment, and in a stroke, 1.9 million brain cells are lost per minute. Your job as the bystander is to have this information packaged and ready. We use a tool called SBAR (Situation, Background, Assessment, Recommendation). You can use a simplified version to be the most helpful person on scene.
The single most important piece of information you can give us for a stroke patient is the “Last Known Normal” time. This is not an exaggeration. It is the most critical data point we have. It means the exact time (to the minute, if possible) that the patient was last seen acting completely normal. This determines their eligibility for clot-busting drugs (tPA) and other interventions, which are highly time-sensitive. A vague “he was fine this morning” is useless. “He was fine at 9:15 AM when he was on the phone, and I found him like this at 9:30 AM” is gold. This is the information that dictates our entire treatment pathway, and a recent 2024 systematic review found a 40% higher odds of excellent functional outcomes when treated within the golden hour.
After the Last Known Normal time, we need a quick background: major medical conditions (especially diabetes, atrial fibrillation, or a history of previous strokes) and a list of medications. Specifically, we need to know if they are on any blood thinners like Warfarin, Eliquis, Xarelto, or Plavix. This is non-negotiable information. A great tip is to have your elderly loved ones take photos of their medication bottles and keep them in a dedicated album on their phone. In an emergency, this is infinitely faster than trying to round up bottles from a medicine cabinet.
Your Checklist: Paramedic Priority Information (SBAR)
- Situation (Most Critical): State the ‘Last Known Normal’ time. The exact time the patient was last seen without symptoms. Write it on a piece of paper for us.
- Background (Medical): List known major medical conditions. Focus on diabetes, high blood pressure, atrial fibrillation (AFib), and any history of prior strokes or heart attacks.
- Background (Medications): Hand over a medication list or the patient’s phone with photos of the bottles. Specifically, point out any blood thinners (anticoagulants/antiplatelets).
- Assessment (What You Saw): Briefly describe the specific symptoms you observed (e.g., “Left-sided face droop started first, then speech became slurred.”).
- Assessment (What You Did): Report any actions taken. “CPR was started at 10:05 AM,” “One 325mg aspirin was chewed at 10:07 AM,” or “An AED was used once.”
Why Chest Pain Always Trumps A Broken Arm In Triage?
In an emergency room or at a mass casualty incident, we operate on a principle called triage. Triage is the brutal but necessary process of prioritizing patients based on the severity of their condition. It’s not about who is in the most pain or who arrived first; it’s about who is most likely to die without immediate intervention. This is why a person with severe chest pain will always be seen before a person with a painfully broken arm. We are governed by the principle of “Life over Limb.”
The core of this triage system is the ABC assessment: Airway, Breathing, and Circulation. A threat to any of these three is a threat to life itself and immediately moves a patient to the top of the list. A broken arm is extremely painful (a limb issue), but it does not typically threaten the ABCs. Chest pain, however, is a direct and immediate potential threat to Circulation. It signals a possible heart attack, which can stop the heart from pumping blood to the brain and other vital organs. An obstructed airway, inability to breathe, or a failing circulatory system will kill a person in minutes. A broken bone will not.
This same logic applies to your actions as a first responder. If you have one person with stroke symptoms (a threat to Circulation in the brain) and another who has fallen and broken their arm, your priority is the stroke patient. It may seem counterintuitive, especially if the person with the broken arm is screaming in pain and the stroke patient is quiet and confused. But your job is to apply the triage mindset: identify and act on the greatest threat to life first. Understanding this principle also helps manage anxiety in a crowded ER; if you are waiting, it’s often a good sign that the medical team has triaged you as stable enough to wait.
Your Checklist: The ABC Priority System
- A – Airway: Is the person’s airway open and clear? A blocked airway (e.g., from choking or swelling) is the most immediate threat to life and must be addressed in seconds.
- B – Breathing: Is the person breathing effectively? Inadequate or absent breathing is the second-highest priority as it cuts off oxygen to the body.
- C – Circulation: Does the person have a pulse? Is there severe, uncontrolled bleeding? Issues with circulation, like a heart attack or cardiac arrest, are the third-highest priority.
- Life over Limb Principle: Remember that any threat to Airway, Breathing, or Circulation will always be prioritized over injuries to extremities (limbs), no matter how painful or visually dramatic they are.
- Dynamic Triage: Patient conditions can change. Always be prepared to reassess the ABCs. A stable patient can become unstable, changing their priority level.
Why Confusing A Heart Attack With Cardiac Arrest Delays The Right Response?
This is one of the most common and dangerous points of confusion for the public. “Heart attack” and “cardiac arrest” are used interchangeably, but they are fundamentally different events requiring completely different immediate responses. Confusing them wastes precious seconds when it matters most.
Think of it this way: a heart attack is a “plumbing” problem. A blockage in a coronary artery is stopping blood flow to a part of the heart muscle. The heart is still beating, but it’s being damaged. The person is typically AWAKE and conscious, complaining of chest pain, shortness of breath, or nausea. Your job for a heart attack is to call 911, keep them calm, and consider giving aspirin.
A sudden cardiac arrest is an “electrical” problem. The heart’s electrical system malfunctions, causing it to stop beating effectively. It quivers or stops entirely. Blood flow to the brain ceases. The person is UNCONSCIOUS, not breathing, and has no pulse. They will collapse suddenly. A heart attack can *lead* to a cardiac arrest, but they are not the same event. Your job for cardiac arrest is to call 911, start CPR immediately, and use an AED as soon as possible. Giving aspirin is useless; you need to manually pump the heart and shock it back into rhythm.
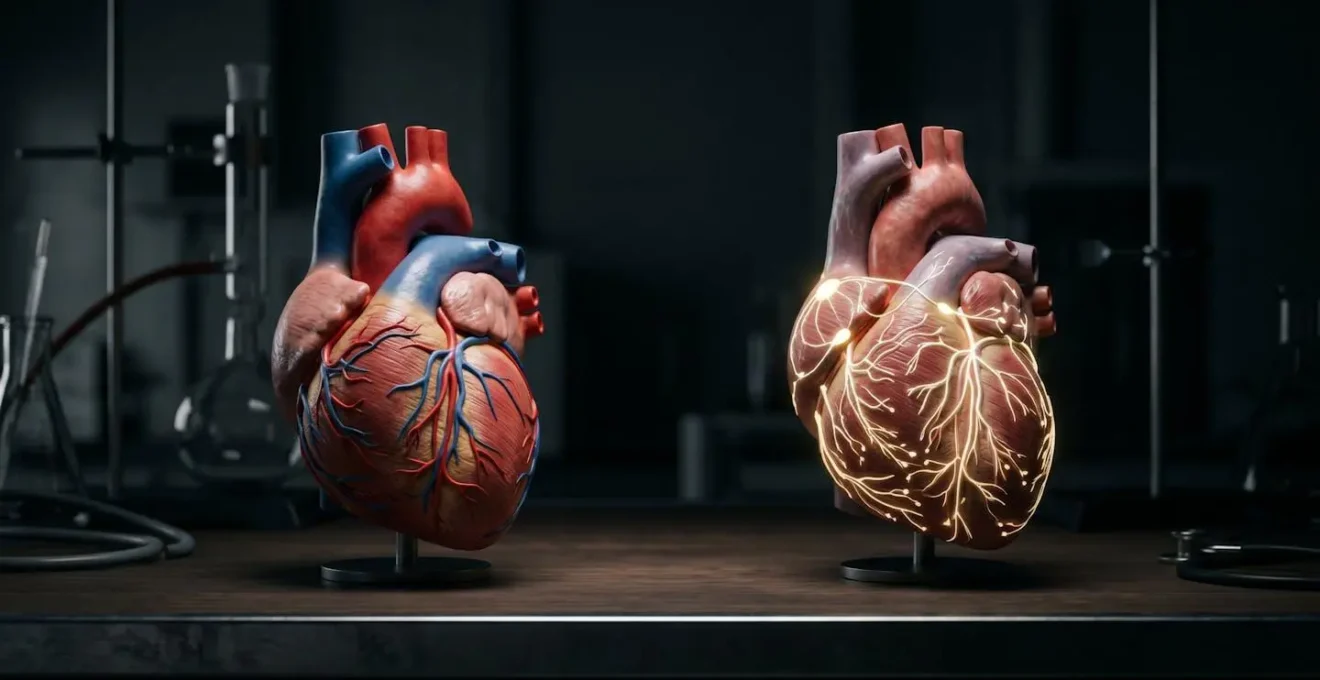
Every second counts. As according to OSHA safety guidelines, there is a 7-10% decrease in survival for each minute that passes without CPR or defibrillation. If you waste time trying to give an unconscious cardiac arrest patient an aspirin, their chances of survival plummet. The correct identification—conscious with chest pain versus unconscious and not breathing—is the first and most important step in the chain of survival.
| Characteristic | Heart Attack (Plumbing Problem) | Cardiac Arrest (Electrical Problem) |
|---|---|---|
| What Happens | Blockage in coronary artery reduces blood flow to heart muscle | Heart’s electrical system malfunctions, heart stops beating effectively |
| Patient Consciousness | Usually AWAKE and breathing | UNCONSCIOUS and NOT breathing |
| Symptoms | Chest pressure, pain radiating to arm/jaw, shortness of breath, nausea | Sudden collapse, no pulse, no breathing, no response |
| Immediate Action | Call 911, keep patient calm, seated, give aspirin if instructed | Call 911, start CPR immediately, use AED as soon as available |
| Aspirin | YES – Chew 325mg non-enteric coated aspirin | NO – Focus on CPR and defibrillation |
Key Takeaways
- Expand your stroke recognition beyond F.A.S.T. to include B.E. for Balance and Eyes, as these are key indicators of often-missed posterior strokes.
- In a crowd, shatter the ‘bystander effect’ by pointing at one person and giving a direct command to call 911, creating accountability and ensuring action.
- The most critical information for a stroke is the ‘Last Known Normal’ time. For cardiac arrest, the critical actions are immediate CPR and using an AED.
How To Use An AED To Save A Life Before The Ambulance Arrives?
An Automated External Defibrillator (AED) is a medical marvel. It’s a device designed to be used by anyone, with or without training, to shock a heart out of a lethal rhythm during sudden cardiac arrest. These devices are found in airports, malls, gyms, and office buildings. Knowing how to use one before we arrive can literally be the difference between life and death. The data is clear: according to the American Heart Association, there is an up to 90% survival rate when defibrillation is achieved within the first minute. That window closes fast.
The most important thing to know about an AED is that you cannot hurt someone with it. The device is intelligent. It will only advise and deliver a shock if it detects a shockable heart rhythm (like ventricular fibrillation). It will not shock a person who has a normal heartbeat or no heartbeat at all (asystole). Fear of making a mistake should never prevent you from using an AED on someone who is unconscious and not breathing.
As soon as someone is assigned to call 911, another person should be sent to retrieve the AED. Once it arrives, open it and the device will begin speaking to you, giving you clear, step-by-step instructions. Your only job is to follow its voice prompts calmly and quickly. While one person operates the AED, another should continue high-quality chest compressions until the AED instructs you to stop. This combination of CPR and early defibrillation is the cornerstone of surviving a sudden cardiac arrest.
Action Plan: Using an AED in 5 Steps
- Turn it On and Expose the Chest: As soon as the AED arrives, turn it on. Immediately remove or cut away the patient’s clothing to expose their bare chest. The area must be dry.
- Apply the Pads: The pads have pictures on them showing exactly where to place them. One pad goes on the upper right side of the chest, the other on the lower left side. Press them down firmly.
- Plug In and Analyze: Plug the pad connector into the AED, usually next to a flashing light. The AED will then say “Analyzing heart rhythm, do not touch the patient.” Ensure no one is touching the person.
- Clear and Shock: If a shock is needed, the AED will charge and then tell you to press the shock button. Before pressing it, loudly command “Everybody clear!” and visually check that no one is in contact with the patient. Then, press the button.
- Resume CPR: After the shock is delivered, the AED will instruct you to resume chest compressions immediately. Continue CPR until the paramedics arrive or the AED tells you to stop for another analysis.
You now possess the core knowledge to act decisively and effectively in a medical crisis. You know how to spot the subtle signs, how to command a scene, and how to communicate with professionals. The next step is to make this knowledge second nature. Mentally rehearse these protocols, locate the AEDs in your workplace and community, and share this information with your family. Be the person who is ready to act.