
The line between ‘medically necessary’ and ‘cosmetic’ surgery is often a clinical or administrative one, but for the patient, both are essential for restoring identity.
- Reconstruction addresses both functional deficits and the deep psychological impact of trauma or disease by restoring anatomical integrity.
- Proving medical necessity to insurance requires specific, objective documentation like visual field tests or standardized photographs that meet defined clinical thresholds.
Recommendation: Focus not just on what can be fixed, but on the surgical techniques—from autologous tissue flaps to microsurgery—that best restore your unique sense of self and psychosocial function.
For patients facing the aftermath of an accident, a cancer diagnosis, or a congenital condition, the question of surgery is deeply personal. Yet, it quickly becomes a matter of public debate, filtered through the rigid definitions of insurance policies. The world wants to know: is this procedure “medically necessary” or merely “cosmetic”? This binary is a false one. As a plastic and reconstructive surgeon, I have seen firsthand that restoring form is inseparable from restoring function. The very foundation of our specialty is that a person’s appearance is not a vanity project; it is a critical component of their identity and psychological well-being.
The distinction is not about function versus beauty, but about restoration versus enhancement. Reconstructive surgery aims to repair, rebuild, and restore the body to a state of normalcy. It is about giving back what was lost to trauma or disease. This is fundamentally different from cosmetic surgery, which enhances features that are already within the normal range. Board-certified plastic surgeons are trained extensively in both disciplines, but it is the reconstructive foundation that informs our understanding of anatomy, healing, and what it means to make a patient whole again.
This guide moves beyond the simplistic debate. We will explore the profound connection between physical and mental recovery, the objective data required to prove medical necessity, the nuanced choices between different surgical techniques, and the unspoken realities of the reconstructive journey. The goal is not just to fix a part of the body, but to restore a person’s ability to re-engage with their life, unburdened by the physical and emotional weight of their condition.
To navigate this complex landscape, this article breaks down the essential considerations a patient must understand. We will walk through the critical aspects of the reconstructive process, from initial justification to long-term outcomes, providing clarity and empowering you to have informed conversations with your medical team.
Summary: Reconstructive Surgery: A Guide to Restoring Form and Function
- Why Physical Reconstruction Is Crucial For Mental Recovery After Trauma?
- How To Prove Medical Necessity To Insurance For Eyelid Surgery?
- Autologous Tissue or Implants: Which Offers More Natural Results?
- The Revision Rate In Reconstruction That Nobody Talks About
- When To Schedule Reconstruction During Chemo Protocols?
- Muscle or Skin: Which Tissue Transfer Is Best For Covering Open Wounds?
- How To Care For The Biopsy Site To Avoid An Ugly Indentation?
- How Microsurgery Saves Severed Limbs When Standard Repair Fails?
Why Physical Reconstruction Is Crucial For Mental Recovery After Trauma?
The visible scars of trauma are often just the surface of a much deeper wound. A significant physical alteration, whether from an accident, burn, or cancer surgery, fundamentally changes a person’s self-perception and their interaction with the world. This is not about vanity; it is about psychosocial function. The ability to meet someone’s gaze, to feel comfortable in public, or to simply recognize the person in the mirror are functions as essential as a limb’s mobility. When this anatomical integrity is compromised, the psychological toll can be immense, often leading to anxiety, depression, and social isolation.
Research consistently shows that the psychological impact of disfigurement is severe. In fact, approximately 20% of patients develop post-traumatic stress following major surgery and physical trauma. Reconstructive surgery directly intervenes here. By restoring physical normalcy, we provide a foundation for psychological healing. The process of reconstruction is a powerful signal to the patient that their wholeness matters and that recovery is possible. It is an active step toward reclaiming a lost part of their identity.
Case Study: The Significant Psychological Impact of “Minor” Limb Loss
A clinical study highlighted the profound psychological distress caused by what might be considered a minor injury: partial finger amputation. The study followed 25 adult patients, finding that all but one experienced significant psychological symptoms, including depression, anxiety, and PTSD, for at least three months. For many, symptom resolution took over six months. This powerful example, detailed in a study on the consequences of digital amputation, proves that the loss of even a small part of one’s physical self can trigger a psychological response comparable to major limb loss, underscoring the critical need for an approach that addresses both physical and mental recovery.
Therefore, framing reconstruction as “optional” or “cosmetic” fundamentally misunderstands its therapeutic purpose. It is a medically necessary intervention aimed at treating the full scope of a traumatic injury—both the physical defect and the associated psychological distress that prevents a patient from living a full life. Identity restoration is not a side effect of the surgery; it is the primary goal.
How To Prove Medical Necessity To Insurance For Eyelid Surgery?
Eyelid surgery, or blepharoplasty, is a perfect example of a procedure that straddles the line between reconstructive and cosmetic. While often sought for aesthetic rejuvenation, it becomes medically necessary when drooping upper eyelids (ptosis) significantly impair vision. The key to securing insurance coverage is to move from a subjective complaint (“I can’t see well”) to objective, quantifiable proof that meets the insurer’s specific clinical threshold. This requires a systematic and thorough documentation process led by your surgeon and ophthalmologist.
Insurance carriers have strict criteria. For example, they will require a visual field test to demonstrate that the eyelid skin is physically obstructing the superior visual field. This is not a guess; it’s a precise measurement. The test is often repeated with the eyelids taped up to prove that lifting the lids provides a quantifiable improvement in vision. Similarly, photographs are not casual snapshots but standardized medical documents taken from specific angles to measure the Margin Reflex Distance (MRD1)—the distance from the center of the pupil to the edge of the upper eyelid. An MRD1 of 2mm or less at normal gaze is a common threshold that signals a functional problem.
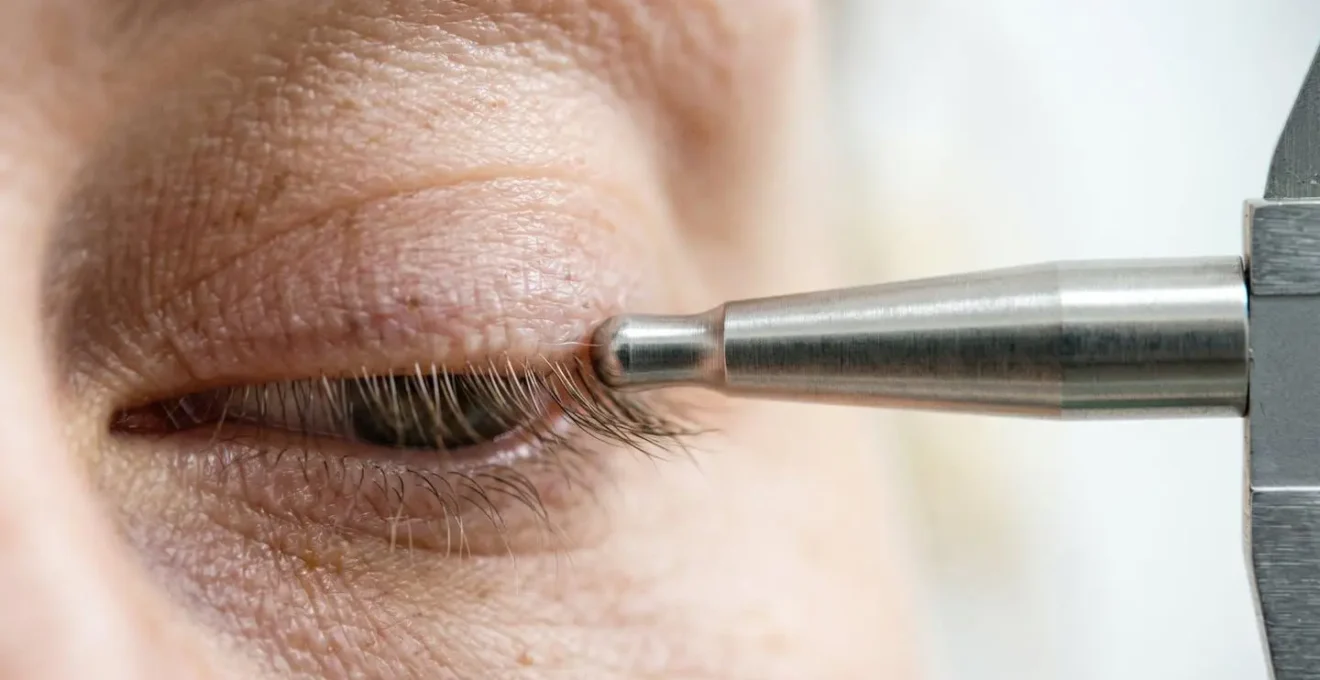
Beyond these tests, a detailed patient history is crucial. Documenting functional impairments such as headaches from constant brow-lifting, neck pain from tilting the head back to see, or difficulty with reading and driving provides essential context. This collection of objective data and subjective experience builds an undeniable case that the surgery is not for looks, but for restoring a fundamental function.
Your Action Plan: Assembling the Evidence for Insurance Approval
- Obtain visual field testing showing superior visual field loss of 30 degrees or less, with documented improvement of 12 degrees or 30% when eyelids are taped.
- Provide standardized photographs taken at eye level, frontal view, with non-dilated eyes, showing the light reflex on the cornea and the lid margins’ position relative to the pupil.
- Document a Margin Reflex Distance (MRD1) measurement of 2mm or less at normal gaze.
- Include a detailed patient diary logging functional impairments like headaches, reading difficulty, or neck pain from compensatory head tilting.
- Ensure your surgeon references specific ICD-10 diagnostic codes for ptosis (H02.401-H02.409) or blepharochalasis (H02.30-H02.36) in the submission.
- Provide a comprehensive medical history demonstrating a full evaluation of the underlying cause and any co-morbidities.
Autologous Tissue or Implants: Which Offers More Natural Results?
One of the most significant decisions in reconstructive surgery, particularly in breast reconstruction after mastectomy, is the choice of material: using the body’s own tissue (autologous reconstruction) or using synthetic implants. While implants offer a more straightforward procedure with faster recovery, the question of “natural results” often leads patients and surgeons toward autologous options. This isn’t just about feel or appearance; it’s about creating a reconstruction that ages, moves, and behaves like the rest of the body—a cornerstone of identity restoration.
Autologous reconstruction involves transferring tissue—typically skin, fat, and sometimes muscle—from one part of the body (like the abdomen, back, or thighs) to the chest to create a new breast mound. The most common procedures are the DIEP flap (from the abdomen) and the latissimus dorsi flap (from the back). Because this is living tissue, it can fluctuate with weight changes, feels warm to the touch, and drapes more naturally over time. This creates a lasting result that requires less long-term maintenance, as there is no risk of implant rupture or the need for replacement surgeries that are often associated with implants.
The “natural” quality of autologous tissue is not merely subjective. It has been validated by research. As a comprehensive review of patient outcomes found, the long-term satisfaction is demonstrably higher with this approach.
Autologous reconstruction yields a higher satisfaction with overall outcome and breast. These findings can aid clinicians when discussing breast reconstruction options with patients.
– Research team from multiple institutions, Systematic review and meta-analysis published in PubMed
However, the choice is not always simple. Autologous procedures are longer, more complex surgeries with a more involved recovery and additional scars at the donor site. The decision depends heavily on a patient’s anatomy, previous surgeries, overall health, and personal goals. For some, the simplicity of an implant-based reconstruction is the right choice. For others, the promise of a more permanent, natural-feeling result that is truly “their own” makes the complexity of an autologous reconstruction a worthwhile journey.
The Revision Rate In Reconstruction That Nobody Talks About
In the narrative of reconstruction, the focus is often on the primary surgery—the one that fixes the initial problem. However, an honest and empathetic discussion must include the topic of revision surgery. A revision is any subsequent procedure performed to improve upon the outcome of the original surgery. It is not necessarily a sign of failure, but rather a reflection of the incredible complexity of working with living, healing tissue. Scars contract, tissues settle, and the body’s healing process can be unpredictable. Setting realistic expectations about the likelihood of needing a “touch-up” is a crucial part of the patient journey.
Revision rates vary dramatically depending on the complexity of the original procedure. For example, a large national database study of 58,264 patients found that for breast reconstruction, revision rates were around 6.2% for autologous reconstructions and just under 4% for implant-based ones within a certain timeframe. These numbers seem low, but they represent thousands of patients returning to the operating room for procedures like scar revision, fat grafting to improve contour, or repositioning an implant. The goal of these revisions is often to achieve better symmetry and a more refined final result—perfecting the functional aesthetics.
Case Study: Rhinoplasty Complexity and Revision Likelihood
Rhinoplasty (a “nose job”) provides a clear example of how complexity correlates with revision rates. A primary septorhinoplasty for a simple cosmetic or functional issue has a relatively low revision rate of around 3.1%. However, as the complexity increases, so does the likelihood of a follow-up procedure. Secondary (revision) rhinoplasty itself carries an 11% re-revision rate. When grafts are required, such as using cartilage from the rib or ear, rates can jump to 21.5%. For the most complex cases, like cleft rhinoplasty, the revision rate is a significant 16-17%. These figures help illustrate that the more variables and challenges involved, the more likely a second stage is needed to achieve the optimal outcome.
Understanding that reconstruction is often a process, not a single event, is vital for a patient’s mental preparation. It shifts the perspective from a one-time fix to a collaborative journey between surgeon and patient, working together over time to achieve the best possible restoration of form and identity. A frank conversation about potential future steps is a sign of a surgeon who respects the patient and the process.
When To Schedule Reconstruction During Chemo Protocols?
For cancer patients, particularly those with breast cancer, the question of timing reconstructive surgery around chemotherapy is a critical and complex one. The decision involves a delicate balance between the oncologic imperative to treat the cancer and the reconstructive goal of restoring form. There is no one-size-fits-all answer; the scheduling is a highly individualized decision made by a multidisciplinary team including the surgeon, oncologist, and the patient.
The primary concern is patient safety. Chemotherapy agents work by targeting rapidly dividing cells—both cancer cells and healthy ones, like those in the bone marrow that produce white blood cells. This leads to immunosuppression and a state called neutropenia, where the body has a severely limited ability to fight infection. Performing a major surgery during a period of profound neutropenia carries a prohibitively high risk of wound healing complications, life-threatening infection, and potential compromise of the reconstruction itself. Therefore, surgery is almost always scheduled to avoid the nadir, or lowest point, of a patient’s blood counts, which typically occurs 7-14 days after a chemo infusion.
There are generally three timing options for reconstruction:
- Immediate Reconstruction: Performed at the same time as the mastectomy, before chemotherapy begins. This is often an option for patients who will receive chemotherapy after surgery.
- Delayed-Immediate Reconstruction: A tissue expander is placed at the time of mastectomy. The expansion process with saline injections may occur during chemo, with the final exchange for a permanent implant or autologous flap happening after all cancer treatments are complete.
- Delayed Reconstruction: No reconstructive steps are taken until after all chemotherapy and radiation treatments are finished, typically waiting at least 3-6 months to allow the body to fully recover.
The best path depends on the specific chemotherapy regimen, whether radiation is needed (which further damages tissue), the patient’s overall health, and their personal preferences. A collaborative approach ensures that the reconstructive plan does not delay or compromise the life-saving cancer treatment.
Muscle or Skin: Which Tissue Transfer Is Best For Covering Open Wounds?
When a surgeon is faced with a large, open wound—perhaps from trauma, tumor removal, or a severe infection—the primary goal is to achieve stable, durable coverage. This is not simply a matter of closing the skin; it is about restoring anatomical integrity and creating a healthy environment for healing. The choice of tissue to accomplish this depends entirely on the nature of the “wound bed.” The two main options are a skin graft or a tissue flap, and understanding the difference is key to understanding modern reconstructive surgery.
A skin graft is essentially a patch. It involves harvesting a thin layer of skin from a healthy donor site on the patient’s body and laying it over a clean, well-vascularized wound bed. It’s like laying sod on prepared soil; the graft has no blood supply of its own and must pick one up from the bed below to survive. This works well for shallow wounds with healthy underlying tissue, like a burn or a skin cancer excision site on the leg.
A tissue flap, by contrast, is a more robust solution. It is a unit of tissue that is transferred with its own blood supply intact. A flap can be composed of skin, fat, muscle, or even bone. Because it brings its own blood supply (an artery and a vein), it can survive on a wound bed that has poor circulation, such as exposed bone, tendon, or a previously irradiated area. A muscle flap, for example, is excellent for filling deep, complex defects. It provides bulky, vascularized tissue that is highly resistant to infection and creates a healthy, padded surface over which a skin graft can then be placed. The choice isn’t “muscle or skin,” but rather determining if the wound needs a simple patch (skin graft) or a life-support system (a vascularized flap).
How To Care For The Biopsy Site To Avoid An Ugly Indentation?
A biopsy is a minor procedure, but the resulting scar can be a major source of concern for patients. One of the most common complaints is the development of a “divot” or indentation at the biopsy site, particularly after a shave or punch biopsy on the face, arms, or legs. This depression occurs due to the loss of subcutaneous tissue (the fatty layer beneath the skin) and the scar tissue tethering the skin surface down. While some degree of scarring is inevitable, proper wound care and technique can significantly minimize the risk of an unsightly indentation, preserving the area’s functional aesthetics.
The process starts with the surgeon. Achieving a tension-free closure is paramount. If sutures are used, a layered closure that carefully re-approximates the deeper tissue layers before closing the skin can help support the surface and prevent it from sinking. For open wounds left to heal on their own, the post-procedure care is in the patient’s hands and is equally critical. The primary goals are to keep the wound moist, clean, and protected.
Here are the key steps to promote optimal healing:
- Keep it Moist: A healing wound should be covered with a petroleum-based ointment (like Vaseline or Aquaphor) and a bandage. This creates a moist environment that prevents scab formation. Scabs impede healing and can increase scarring.
- Keep it Clean: Gently cleanse the area daily with mild soap and water. Avoid harsh antiseptics like hydrogen peroxide or alcohol, which can damage delicate healing tissue.
- Pressure and Massage: Once the wound is fully closed, gentle pressure and scar massage can help break down collagen and soften the scar, preventing it from becoming hard and tethered. Silicone sheets or gels are also highly effective at this stage, as they hydrate the scar and reduce excessive collagen buildup.
- Sun Protection: A new scar is highly susceptible to sun damage, which can cause it to become permanently hyperpigmented (darkened). Meticulous sun protection with a broad-spectrum SPF 50 sunscreen for at least one year is non-negotiable.
By following these steps, you actively participate in the healing process, giving your body the best possible chance to create a smooth, flat, and minimally visible scar.
Key Takeaways
- Physical reconstruction is a medical necessity for mental health, as restoring anatomical form is crucial for reclaiming a patient’s sense of identity after trauma.
- Securing insurance approval depends on providing objective, quantifiable data—like visual field tests or standardized measurements—that meet specific clinical thresholds for functional impairment.
- The ultimate goal of reconstruction is not just to repair a defect but to restore wholeness, and the likelihood of revision surgery should be seen as part of a meticulous, multi-stage process toward that goal.
How Microsurgery Saves Severed Limbs When Standard Repair Fails?
In the world of reconstructive surgery, few things represent the pinnacle of technical skill and life-altering impact like microsurgery. This is the specialized field that allows surgeons to operate on structures so small they are barely visible to the naked eye. When a limb or digit is severed in a traumatic accident, standard surgical repair is often impossible. The arteries, veins, and nerves are simply too small to be reconnected with conventional instruments and techniques. This is where microsurgery becomes the difference between a successful replantation and an amputation.
Microsurgery is performed using a high-powered operating microscope that magnifies the surgical field up to 40 times. Surgeons use exquisitely fine instruments—sutures thinner than a human hair and needles that are barely perceptible—to perform a re-anastomosis, the meticulous reconnection of severed vessels and nerves. The first and most critical step is restoring blood flow. The surgeon must successfully repair at least one artery to bring oxygenated blood into the limb and at least two veins to carry blood out. Failure on either side leads to the death of the replanted part.
Once circulation is re-established, attention turns to the nerves. Repairing a severed nerve is like splicing thousands of tiny telephone wires. A successful nerve repair is what will eventually allow for the return of sensation and motor function, a process that can take months or even years as the nerves slowly regenerate. This is the ultimate act of identity restoration—giving back not just the form of a hand, but the ability to feel a loved one’s touch or the dexterity to return to a cherished hobby. While not every severed limb can be saved, microsurgery has transformed what is possible, pushing the boundaries of reconstruction and offering hope in the most devastating of circumstances.
Ultimately, the decision to undergo reconstructive surgery is a collaborative one. If you are considering a procedure, the most important step is to seek a consultation with a board-certified plastic surgeon who understands this holistic approach—one who sees you not as a collection of parts to be fixed, but as a whole person seeking to restore your life. They can provide a thorough evaluation and guide you toward the options that will best achieve your functional and personal goals.