
When you’re admitted to the hospital, all focus tends to gravitate toward the surgeon’s hands or the specialist’s diagnosis. We are conditioned to see doctors as the sole drivers of our recovery. We obsess over their brief visits, hang on their every word, and see the time in between as simple, passive waiting. This is a dangerous misconception. The reality of your safety and the quality of your recovery is forged not in the 15-minute doctor’s round, but in the countless hours spent with the person at your bedside: your clinical nurse.
The common understanding is that nurses are there to provide comfort and administer medications. While true, this view is woefully incomplete. It misses their most critical function. Your nurse is the central processing unit of your hospital care. They are the vigilant sentinel watching for subtle changes, the skilled negotiator translating your needs into clinical action, and the final safety net protecting you from a complex and sometimes fractured system. They are your most powerful advocate, but this advocacy is not automatic. It is a partnership, and you are the other half of the equation.
But what if the key to a safer, faster recovery wasn’t just hoping for a “good nurse,” but knowing how to be a “good patient-partner”? This guide is written from decades of experience on the ward. It’s not about being demanding; it’s about being effective. We will bypass the platitudes and give you the specific, actionable intelligence you need. You will learn why nurse staffing is a personal safety issue, how to communicate your pain to get real results, how to become the final checkpoint against medication errors, and how to leverage your nurse’s deep knowledge to ensure you leave the hospital and stay out.
This guide provides a clear roadmap for navigating your hospital stay. Each section tackles a critical aspect of the nurse-patient partnership, empowering you with the knowledge to transform from a passive recipient of care into an active participant in your own recovery.
Summary: Why Your Clinical Nurse Is Your Most Important Recovery Partner
- Why Understaffed Wards Increase Infection Risks By 40%?
- How To Report Pain Levels To Get The Right Medication Faster?
- RN or NP: Who Can Prescribe Your Discharge Meds?
- The Bedside Check That Prevents 90% Of Drug Administration Errors
- How To Use Your Nurse’s Knowledge To Prevent Readmission?
- How To Describe Pain Intensity Without Exaggerating?
- Why Seeing Your Doctor Use Sanitizer Is Not Always Enough?
- How To Navigate Clinical Workflows To Reduce Your ER Wait Time?
Why understaffed wards increase infection risks by 40%?
The number of patients assigned to your nurse is not an abstract administrative metric; it is a direct and powerful predictor of your personal safety. When a nurse is stretched too thin, their ability to perform meticulous, consistent infection control is the first casualty. They have less time for thorough hand hygiene between patients, for systematically disinfecting shared equipment, or for carefully managing invasive lines and catheters. This isn’t about a lack of care or skill; it’s a simple, brutal equation of time and attention. Every additional patient dilutes the vigilance that keeps you safe from hospital-acquired infections (HAIs).
The data is frighteningly clear. Overstretched nursing staff is a recipe for preventable harm. Comprehensive research demonstrates that inadequate staffing has dramatic consequences, correlating higher nurse-to-patient ratios with significant increases in central line bloodstream infections, catheter-associated urinary tract infections, and ventilator-associated pneumonia. Your risk isn’t theoretical; it’s a statistical probability that rises with every new admission to an already busy ward. Being a patient in an understaffed environment means you must become a more vigilant co-manager of your own safety.
Case Study: The Direct Link Between Staffing and COVID-19 Infection
A landmark 2025 retrospective cohort study during the COVID-19 pandemic provided a stark illustration of this principle. Examining over 67,000 cases in South Korean hospitals, researchers found that as nurse-to-patient ratios worsened, the rate of patients contracting COVID-19 *after* admission skyrocketed. The data showed that when staffing levels were compromised, essential infection control protocols failed, leading to an alarming 15.1% of patients in general wards becoming infected in the hospital. This study proves that a nurse’s workload translates directly into your risk of a preventable, in-hospital infection.
You have a right to ask about the staffing on your unit. While you cannot change it, being aware of the situation allows you to elevate your own vigilance. Pay closer attention to hygiene practices, question procedures, and understand that you may need to be a more proactive advocate for your own care when the system itself is under strain.
How to report pain levels to get the right medication faster?
“I’m in pain.” It’s the most common report a nurse hears, but it’s also one of the least useful. Vague descriptions lead to a frustrating cycle of trial-and-error medication, with you suffering in the meantime. To get the right relief faster, you must shift from being a passive reporter of discomfort to an active communicator of data. Your nurse needs specific information to differentiate between nerve, muscle, or inflammatory pain, and to understand how it’s affecting your ability to function. They are your system interface to the pharmacy, but they need the right input.
Clinicians use a framework called “PQRST” to assess pain, and you can use it to structure your report for maximum impact. Instead of waiting to be asked, present your pain using these categories. This proactive communication demonstrates that you are an engaged partner and gives your nurse the precise details needed to advocate for the most effective treatment from the prescribing doctor. This is not about complaining; it’s about providing a high-quality clinical report.
This structured approach helps your nurse understand the full picture. The goal is not just to lower a number on a scale, but to restore function—to allow you to breathe deeply, get out of bed, or focus on a conversation. When you provide this level of detail, you empower your nurse to get you the right medication, at the right dose, for the right type of pain.
Here’s how to structure your communication using the PQRST framework to get the best results:
- P – Provocation/Palliation: “The pain gets worse when I try to sit up, but it feels a little better if I lie flat on my back.”
- Q – Quality: Use descriptive words. “It’s not a dull ache; it’s a sharp, stabbing feeling on the right side.”
- R – Region/Radiation: Be precise. “It starts right here (point with one finger) and seems to shoot down my leg.”
- S – Severity: Connect the number to your function. “I’d call it a 7 out of 10, which means I can’t even focus on watching TV.”
- T – Timing: Describe the pattern. “It’s been constant for the last two hours, and the last dose of pain medication only helped for about an hour.”
RN or NP: who can prescribe your discharge meds?
As your hospital stay nears its end, a flurry of activity begins around your discharge plan. One of the most critical components is your list of prescriptions. A common point of confusion for patients is who, exactly, has the authority to make these decisions. Legally, the authority to write prescriptions rests with licensed prescribers: doctors (MDs, DOs), and in many settings, advanced practice nurses like Nurse Practitioners (NPs) or Physician Assistants (PAs). A bedside Registered Nurse (RN) cannot, by law, write a prescription.
However, to believe the RN has no influence here is a grave mistake. The bedside RN is the single most important source of real-world information that shapes what is ultimately prescribed. They are the ones who know you can’t swallow large pills, that you live alone and can’t manage complex insulin injections, or that you don’t have the financial means for a brand-name drug. They perform the critical “reality check” on the doctor’s or NP’s plan. They are your advocacy leverage in the crucial moments before the prescription is finalized.
This distinction is vital. While the NP or doctor holds the prescription pad, their decisions are heavily guided by the RN’s detailed assessment. As nursing care professionals from Shaker Place note in their analysis on holistic recovery:
While an NP or doctor writes the prescription, the bedside RN’s assessment of practical barriers heavily influences what is ultimately prescribed.
– Nursing care professionals, Nursing care services and holistic patient care analysis
Therefore, your strategy should be to communicate any practical concerns about your future medications directly to your RN. Tell them, “I’m worried about affording this,” or “I have trouble remembering to take pills three times a day.” Your RN can then take this crucial information to the prescriber to find a medication regimen that is not just clinically appropriate, but also practical for you to follow at home. This is how you prevent medication non-adherence and potential readmission before you even leave the hospital.
The bedside check that prevents 90% of drug administration errors
The single most dangerous moment in a hospital is often the most routine: the administration of medication. While the system has numerous checks, errors can and do happen. The final, and most important, safety check is you. By being an active, informed participant, you can help your nurse prevent a potentially life-threatening mistake. This isn’t about distrust; it’s about partnership. It’s about performing your role in the system vigilance that ensures your safety. The process is built on a foundation known as the “Five Rights” of medication administration.
Your role is to politely and consistently verify these rights with your nurse every single time you are given a medication. Think of it as a pre-flight checklist for your body. Many hospitals now use barcode scanners to automate parts of this process, but technology is not infallible. Your active participation is the ultimate backup. Voicing a simple question like, “Can you just remind me what this one is for?” can be the action that intercepts an error before it reaches you.
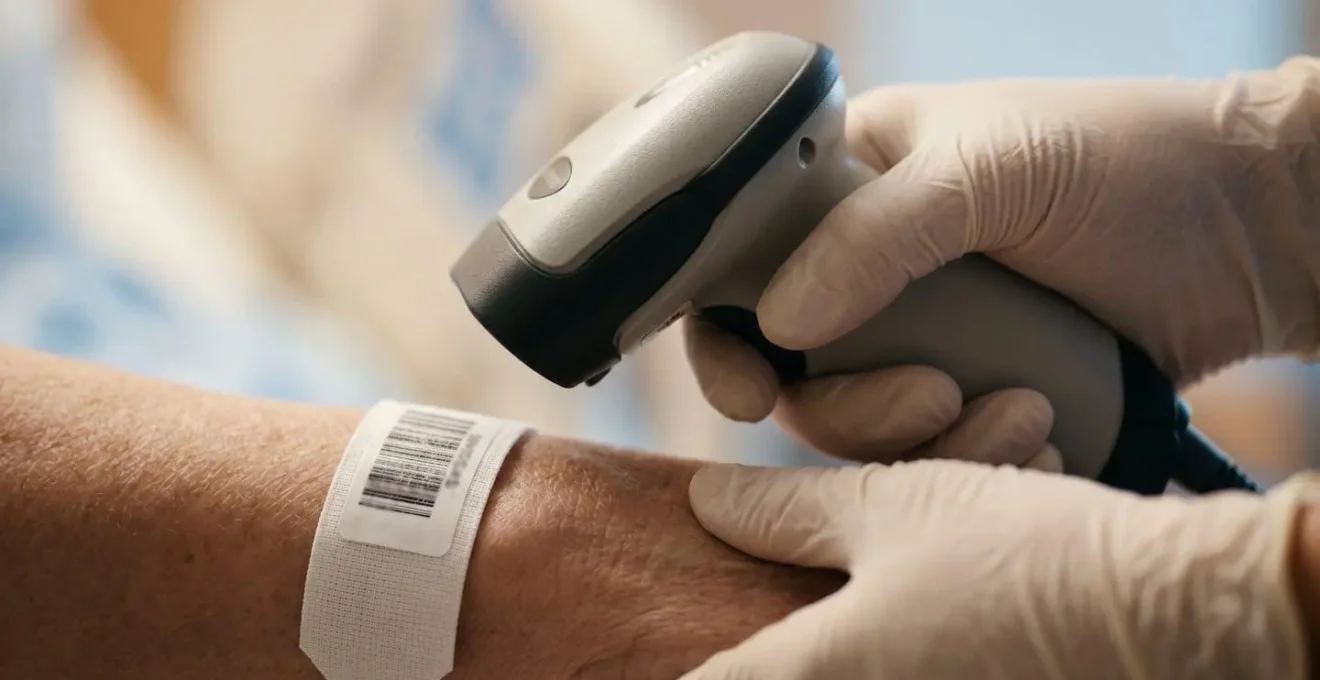
As the image above illustrates, modern safety protocols often involve technology like barcode scanning to confirm your identity. But you are the only one who knows your treatment plan intimately. If a pill looks different, or the timing feels off, speak up immediately. A good nurse will welcome your question. They will see it not as a challenge to their authority, but as a sign of an engaged patient-partner committed to a safe outcome. Your voice is a critical tool in your own protection.
Use this checklist, based on the clinical standard from the National Center for Biotechnology Information (NCBI), as your guide for every medication event:
- Right Patient: Ask the nurse to scan your wristband and verbally confirm your full name and date of birth. Don’t let anyone bypass this step.
- Right Drug: Ask, “What is this medication for?” and confirm it matches what you expect to receive for your condition.
- Right Dose: If a pill looks different in color or size, or if you’re receiving a different number of pills, ask the nurse to double-check the dose. Say, “This looks different from what I got this morning, can we verify it?”
- Right Route: Confirm the method of administration. If you’re expecting a pill and the nurse arrives with a syringe, stop the process and ask for clarification.
- Right Time: If your medication arrives at an unusual hour, ask if the schedule has been officially changed. Timing is crucial for effectiveness and safety.
How to use your nurse’s knowledge to prevent readmission?
Discharge from the hospital is not the end of your recovery; it is the beginning of the most vulnerable phase. The majority of hospital readmissions are not caused by new diseases, but by a failure to properly manage the original condition at home. This often stems from a simple knowledge gap between the hospital’s instructions and the patient’s real-world understanding. Your nurse is the bridge over that gap. Their primary goal at discharge is to transfer their knowledge to you, but you must be an active student.
The single most powerful technique to ensure you understand your care plan is called “Teach-Back.” It’s simple: after your nurse explains your instructions, you repeat them back in your own words. This isn’t a test of your memory; it’s a tool to identify misunderstandings before they become dangerous mistakes at home. Saying, “Okay, so just to make sure I’ve got this right, you want me to…” is the most effective way to take control of your discharge education.
Beyond Teach-Back, your nurse’s experience is a goldmine of preventative knowledge. They have seen hundreds of patients with your condition and know the common pitfalls that lead to readmission. Your job is to extract that wisdom. Be a journalist investigating your own health. Ask targeted questions that go beyond the standard discharge sheet. You are transitioning from patient to co-manager of your health, and this is your final, critical briefing with your expert consultant.
Your Discharge Readiness Checklist: Questions to Ask Your Nurse
- Practice Teach-Back: When your nurse explains your care plan, repeat it back in your own words to identify knowledge gaps before leaving the hospital.
- Create a Red Flag Checklist: Work with your nurse to write down specific symptoms that require calling your doctor versus going to the emergency room.
- Ask ‘What is the most common reason a person with my condition gets readmitted?’ to focus your attention on the highest-risk complications.
- Inquire ‘What should I do if I experience [specific side effect from your medication]?’ to have a concrete action plan for common scenarios.
- Request equipment verification: Ensure you have working tools at home (scale, blood pressure cuff) that your nurse can demonstrate during discharge teaching.
How to describe pain intensity without exaggerating?
The 0-10 pain scale seems simple, but it’s a flawed tool when used in isolation. A “10” for one person might be a “6” for another. The fear of being seen as “drug-seeking” or exaggerating can lead patients to downplay their pain, while others may inflate the number hoping for a faster response. Both approaches are counterproductive. The key to being taken seriously is not to focus on the number itself, but on what that number *means* for your ability to function. Your goal is to provide objective evidence of your pain’s impact.
Instead of just saying “it’s an 8,” translate that number into a functional deficit. For example: “It’s an 8, and at this level, I can’t take a deep breath without sharp pain.” Or, “I’d call it a 6, which for me means I can’t concentrate enough to read or hold a conversation.” This approach gives your nurse concrete, observable data. It moves the conversation from a subjective and easily dismissed number to an objective problem that needs solving. It allows them to document “patient unable to perform deep breathing exercises due to pain,” which is a much stronger justification for intervention than “patient reports 8/10 pain.”
It’s crucial to remember that your experience of pain is valid. As clinical nursing educators emphasize, the definition of pain is fundamentally patient-centered. As they state in their guide to pain assessment:
Pain is whatever the patient says it is. Everyone experiences pain differently and has varying pain tolerances, which is another reason why using the PQRST tool and diving deeper into the patient’s pain matters.
– Clinical nursing educators, PQRST: An Essential Guide to Comprehensive Pain Assessment
This principle empowers you. Your report is the truth. The challenge isn’t to justify the feeling, but to articulate its impact. By tying the subjective number to an objective functional limitation, you provide your nurse with the powerful combination of data and context they need to advocate effectively on your behalf and get you the relief you need to recover.
Why seeing your doctor use sanitizer is not always enough?
Hand hygiene is the cornerstone of infection prevention, and seeing a clinician use hand sanitizer before touching you is a reassuring sight. However, it’s only one link in the chain of infection control. Relying on this single action as a guarantee of safety is a mistake. Pathogens are opportunistic and travel on a multitude of surfaces that move from room to room. Your system vigilance as a patient means being aware of these other potential vectors of transmission.
Consider the clinician’s stethoscope. Is it wiped down with an alcohol swab before it touches your skin? What about their necktie, sleeves, or the portable blood pressure cuff that was just used on the patient next door? These items, known as “fomites,” can easily carry bacteria and viruses. While nurses are often highly trained in managing this risk, the fast-paced hospital environment can lead to lapses. Your gentle awareness and polite questions can serve as a crucial reminder.
You have the right to a clean environment and clean equipment. You can politely ask, “Would you mind wiping that down before you use it?” when a piece of shared equipment is brought to your bedside. This is not an accusation; it’s a collaborative act of safety. You are reinforcing the hospital’s own protocols and acting as a partner in preventing a healthcare-associated infection. A professional clinician will respect this and see it as a sign of an informed, engaged patient. True safety goes beyond just clean hands; it requires a culture of cleanliness for every object and surface that enters your personal space.
Key Takeaways
- Your bedside nurse is your most critical partner; their workload directly impacts your safety and your communication with them dictates your outcomes.
- Use structured communication frameworks like PQRST for pain and Teach-Back for discharge to prevent errors and misunderstandings.
- You are the final safety check. Actively participate in verifying medications and observing infection control to protect yourself.
How to navigate clinical workflows to reduce your ER wait time?
The Emergency Room (ER) is not a first-come, first-served environment. It’s a high-stakes sorting system where patients are prioritized based on the severity of their condition. Your wait time is determined by a triage nurse who uses a system like the Emergency Severity Index (ESI) to decide how quickly you need to be seen. Understanding this allows you to communicate more effectively and potentially reduce your wait. The key is to provide the triage nurse with a concise, high-impact report that contains the keywords they are trained to listen for.
Your first 30 seconds with the triage nurse are the most important. You must act as the “executive summary” of your own medical crisis. State your chief complaint clearly, followed by any critical vital signs and relevant history. This is not the time for a long, meandering story. It’s a data transfer. Using words like “chest pain,” “shortness of breath,” or “sudden severe headache” immediately elevates your priority. This isn’t about manipulation; it’s about using the correct clinical language to ensure your situation is accurately assessed by your primary nurse as the system interface.
Preparing an “ER Ready Packet” with your medication list, allergies, and medical history can save critical time and prevent errors when you are least able to communicate clearly. Handing this directly to the triage nurse allows them to quickly input your data and move on to their assessment. By being organized and precise, you help the system work more efficiently for you. You are demonstrating that you understand the process and are a partner in your own care, even in a high-stress environment.
To give the triage nurse the best possible information, follow this communication strategy:
- Prepare a 30-second summary: Start with the most critical information. “I’m here for chest pain. It started an hour ago. I have a history of high blood pressure.”
- Use priority-escalating keywords: Clearly state symptoms like ‘chest pain,’ ‘shortness of breath,’ ‘sudden severe headache,’ or ‘fever in an infant under 3 months’ as these are clinical red flags.
- Create an ‘ER Ready Packet’: Keep a card or phone note with your medications, allergies, emergency contacts, and major medical history to hand directly to the nurse.
- Be specific about timing and changes: “This headache started 2 hours ago and is much worse than my usual migraines.”
- Ask the triage nurse directly: Politely ask, “Based on my symptoms, what is the approximate wait time I should expect?” This helps manage your own expectations.
Now that you are armed with this knowledge, your role is clear. The next time you or a loved one is in the hospital, do not be a passive bystander. Be a prepared, informed, and respectful partner. Use these strategies to communicate with your nurse, participate in your care, and actively build the partnership that is most critical to your recovery.